Continuous glucose monitors were once reserved for diabetes management, but a growing wave of CGM systems now targets metabolic health enthusiasts, athletes, and anyone curious about how food, sleep, and exercise influence their blood sugar. These devices promise real-time insight into glucose patterns - data that traditional finger-prick monitors capture only as snapshots.
Before committing to a sensor subscription or ordering your first device, it helps to understand five decision criteria: who stands to benefit most from continuous tracking, what the data actually measures and reveals, how to interpret glucose curves without clinical training, the cost and access tradeoffs compared to traditional monitors, and when a simpler, on-demand glucose meter may be sufficient for your goals.
This guide walks through each criterion in plain terms, comparing continuous and traditional glucose monitoring where the distinctions matter. It is not medical advice - anyone with diabetes, prediabetes, or metabolic concerns should consult a healthcare provider before choosing or interpreting any glucose monitor. For everyone else exploring wellness tracking, the sections ahead clarify what to expect, what to spend, and how to decide whether a CGM fits your routine.
Who Should Consider a CGM for Wellness Tracking
A continuous glucose monitor can provide helpful feedback for specific wellness goals, but it's not the right fit for everyone. The technology delivers the most value when you have clear objectives and plan to act on the data you collect.
Athletes and active individuals experimenting with fueling strategies often find CGMs useful for understanding how different meals affect energy levels and recovery. By observing glucose responses to pre-workout carbohydrates or post-exercise meals, you can refine timing and composition to support performance without relying on guesswork.
People exploring metabolic flexibility - the body's ability to switch between burning glucose and fat - use CGMs to track how their glucose levels stabilize or fluctuate across different eating patterns. This includes those experimenting with lower-carbohydrate diets, intermittent fasting, or time-restricted eating windows.
If you've been told you have prediabetic markers such as elevated fasting glucose or HbA1c in the high-normal range, a CGM offers objective feedback on how lifestyle changes influence your glucose patterns throughout the day. This visibility can make adjustments to diet, activity, and sleep feel more concrete and measurable.
Individuals curious about how specific foods - such as pasta, fruit, or breakfast combinations - impact their glucose may benefit from short-term CGM use. Seeing your own response curves can clarify which meals lead to steady energy and which cause rapid spikes and crashes.
On the other hand, casual curiosity without a specific goal may not justify the ongoing cost or the attention required to interpret the data. CGMs generate a continuous stream of information, and without a framework for using it, the numbers can feel overwhelming or lead to unnecessary worry over normal glucose fluctuations.
Consider whether you're ready to adjust habits based on what you learn. If you're not planning to change your diet, activity, or sleep in response to glucose trends, the device may add complexity without delivering meaningful benefits.
What CGMs Actually Measure and What They Don't
Continuous glucose monitors measure glucose levels in the interstitial fluid - the liquid surrounding your cells - rather than directly sampling blood. A small filament sits just beneath the skin and detects glucose that has diffused out of capillaries. Because this transfer takes time, CGM readings typically lag blood glucose by 10 to 15 minutes. During rapid changes, such as immediately after eating or during intense exercise, the sensor reading may not yet reflect what's happening in your bloodstream.
This lag doesn't compromise the device's value for trend tracking. CGMs excel at revealing patterns: the shape and duration of your post-meal glucose curve, the stability of your overnight levels, and how different foods or activities influence your response over hours. You can observe whether a high-protein breakfast keeps your glucose steadier than a carbohydrate-heavy one, or whether an evening walk blunts the spike from dinner.
What CGMs do not measure is the underlying physiology driving those patterns. The sensor cannot assess insulin sensitivity, evaluate pancreatic beta-cell function, or diagnose metabolic conditions. A flat glucose curve may reflect good carbohydrate tolerance, but it may also occur in someone with impaired first-phase insulin response who happens to eat low-glycemic foods. Similarly, occasional spikes do not confirm insulin resistance without additional context such as fasting insulin levels or an oral glucose tolerance test.
For non-diabetic users, the data is most useful as a behavioral feedback loop rather than a diagnostic report. Identifying which meals or snacks produce prolonged elevation, which types of exercise help stabilize readings, and how sleep or stress correlate with morning glucose can inform practical adjustments. The system provides visibility into short-term variability, not a comprehensive picture of long-term metabolic health.
Interpreting CGM data requires recognizing the difference between a response and a risk. A glucose reading of 160 mg/dL an hour after a meal may prompt curiosity about portion size or meal composition, but it does not carry the same clinical significance for a non-diabetic individual as it would for someone managing diabetes. Without baseline lab work - hemoglobin A1C, fasting glucose, or lipid panels - context remains limited.
Set expectations around what the technology offers: real-time insight into how your body responds to daily variables, not a substitute for clinical assessment or a definitive measure of metabolic fitness.
How to Choose Between a CGM and a Traditional Glucose Monitor
Choosing between a continuous glucose monitor and a traditional fingerstick meter depends on how often you want to check your glucose, what you plan to do with the data, and your budget.
A CGM delivers glucose readings every few minutes around the clock, building a continuous picture of how your levels rise and fall throughout the day and night. This makes it easier to spot patterns - such as how different meals, exercise timing, or sleep quality affect your glucose - without having to remember to test at specific moments. The tradeoff is cost: most CGMs require a subscription or regular sensor purchases, and each sensor typically lasts 10 to 14 days before replacement.
A traditional glucose meter requires a fingerstick for each reading, so you only capture snapshots at the times you choose to test. This approach costs significantly less upfront and over time, with no subscription and inexpensive test strips. It works well if you want occasional confirmation - for example, testing fasting glucose a few mornings per week or checking after a specific meal - but it won't reveal trends between tests or catch overnight shifts.
If your goal is to understand how your daily habits influence glucose in real time and you're comfortable with the recurring expense, a CGM offers the visibility to make those connections quickly. If you're testing sporadically to confirm general stability or prefer to avoid wearable sensors, a traditional meter provides accurate point-in-time data at a fraction of the cost.
Consider how frequently you want feedback. Continuous data supports tighter behavior loops - seeing a glucose spike within an hour of eating makes it easier to adjust portion sizes or food combinations the next day. Spot checks offer less frequent feedback but may be enough if you're tracking broader trends over weeks rather than optimizing day-to-day decisions.
Common Mistakes to Avoid When Using a CGM for Wellness
Even experienced wellness users can stumble when they start tracking glucose continuously. Understanding common pitfalls helps you use the data more effectively and avoid unnecessary worry.
One of the most frequent mistakes is overreacting to single data points. Glucose fluctuates naturally throughout the day in response to meals, activity, stress, and sleep. A single spike or dip tells you very little - what matters is the pattern over days and weeks. If you see a reading you don't like, resist the urge to change everything immediately. Instead, watch for trends across similar situations.
Another common issue is misinterpreting the lag between interstitial fluid glucose (what CGMs measure) and blood glucose (what fingerstick meters measure). Interstitial readings typically trail blood glucose by 5 to 15 minutes. During rapid changes - like right after eating or during exercise - this lag can make your CGM reading seem off compared to how you feel. This doesn't mean the sensor is wrong; it's measuring a different sample at a slightly different time.
Many people also expect CGM data to diagnose metabolic conditions. A CGM worn for wellness is not a substitute for clinical testing. It can reveal patterns that prompt you to seek medical advice, but it cannot confirm prediabetes, insulin resistance, or other conditions. If you notice concerning trends, discuss them with a healthcare provider who can order appropriate diagnostic tests.
Context matters more than the numbers alone. Hydration status, stress hormones, illness, medication, and even sensor placement can all influence readings. A poorly secured sensor or one placed on a compressed area may produce erratic data. Dehydration can slow glucose clearance, and stress can trigger glucose release even without food. Always interpret your data within the full picture of what's happening in your life.
Finally, don't neglect the basics while focusing on the data. A CGM can help you refine your habits, but it won't replace foundational practices like balanced meals, regular movement, adequate sleep, and stress management. Use the feedback to guide adjustments, not to micromanage every fluctuation or replace sound wellness principles.
How to Interpret CGM Data Without Medical Training
Reading CGM data without a clinical background is manageable when you focus on a few key patterns. Start by observing your fasting glucose - values taken first thing in the morning before eating. For most non-diabetic adults, a stable fasting range falls between 70 and 100 mg/dL. Consistent readings above 100 may warrant a conversation with a healthcare provider.
Next, watch how your glucose responds after meals. A moderate postprandial peak - typically reaching 120 to 140 mg/dL within one to two hours - is normal. What matters as much as the peak itself is how quickly your glucose returns to baseline. A healthy response usually sees levels drop back within two to three hours. Sharp spikes followed by slow recovery, or prolonged elevation, can signal that a particular meal or combination of foods challenges your system.
Correlation is where the real insight lies. Log what you eat, when you exercise, how much you sleep, and any stress events alongside your CGM trace. Over a week or two, patterns emerge: certain carbohydrate sources may cause larger swings, protein and fat can moderate peaks, and a morning walk might flatten your post-breakfast curve. This context transforms raw numbers into actionable feedback.
Track the time it takes for glucose to return to your baseline after a meal. Consistently slow recovery - remaining elevated beyond three hours - may indicate reduced insulin sensitivity or simply that portion sizes or food choices need adjustment. Use this information to experiment with smaller servings, different macronutrient ratios, or meal timing.
While self-interpretation is useful for general wellness, know when to seek professional input. If your fasting glucose consistently sits above 100 mg/dL, if you see unexplained spikes unrelated to food or activity, or if your glucose remains elevated for extended periods without clear cause, consult a doctor or dietitian. A CGM is a monitoring tool, not a diagnostic instrument, and persistent outliers deserve clinical evaluation.
Keep your expectations realistic. Day-to-day variability is normal. Stress, sleep quality, hydration, and even the previous day's activity all influence glucose. Look for trends over weeks, not isolated readings over hours. The goal is to understand your personal response patterns and make incremental, sustainable changes - not to achieve perfect flatline glucose at all times.
Cost Considerations: CGM Sensors vs. Test Strips Over Time
When evaluating continuous glucose monitoring for wellness tracking, understanding the ongoing financial commitment is essential. Unlike one-time purchases, both CGM systems and traditional meters require regular replenishment of consumables, and the cost structures differ significantly.
CGM sensors are the primary recurring expense in a continuous monitoring approach. Most sensors are designed to last 10 to 14 days before requiring replacement. Typical sensor costs range from $50 to over $100 per unit, depending on the brand and whether insurance coverage applies. For non-diabetic users paying out of pocket, this translates to approximately $150 to $300 per month if monitoring continuously. Some CGM platforms also charge monthly app subscription fees ranging from $20 to $40, which provide data analysis, trend reports, and personalized insights.
Traditional blood glucose meters present a different cost model. The meter itself is a one-time purchase, typically priced between $15 and $20 for basic models. The ongoing expense comes from test strips, which are used once per reading and then discarded. Strip pricing varies widely by brand and retailer, often ranging from $0.25 to over $1.00 per strip when purchased in bulk. A user testing twice daily would use approximately 60 strips per month, leading to costs between $15 and $60 monthly, depending on strip pricing. Lancets add minimal additional cost, usually a few dollars per box of 100.
To compare scenarios: someone using a CGM year-round at $200 per month would spend roughly $2,400 annually. A traditional meter user testing twice daily at $0.50 per strip would spend about $360 per year on strips alone. The cost gap widens significantly with continuous use, but narrows if CGM use is limited to short experimental periods rather than ongoing tracking.
For non-diabetic users exploring glucose awareness, a practical middle ground involves time-limited CGM experiments. Wearing a sensor for one or two months to identify patterns around specific foods, exercise routines, or sleep schedules can provide valuable baseline data without long-term expense. Users can then transition to occasional fingerstick monitoring to verify trends or check specific meals, reducing ongoing costs while maintaining awareness.
Budget planning should also account for hidden expenses. CGM adhesive patches, skin prep wipes, and over-patches to secure sensors during workouts or swimming add small but cumulative costs. Traditional meter users may need to replace their device eventually, though most meters last several years with basic care. Neither approach includes potential costs for nutritionist consultations or coaching services, which some users pursue to interpret their glucose data effectively.
The value equation depends heavily on individual goals. Users seeking comprehensive data to optimize athletic performance or manage energy levels throughout the day may find the CGM investment worthwhile despite higher costs. Those simply curious about their glucose response to occasional meals or wanting periodic check-ins may find traditional monitoring more economical and sufficient for their needs. Calculating your expected testing frequency and duration before purchasing helps align your monitoring approach with both your wellness goals and your budget constraints.
Final Takeaway: Match Your Monitoring Method to Your Goals
Choosing between a continuous glucose monitor and traditional fingerstick testing comes down to matching the tool to what you actually want to learn. If your goal is to understand how specific meals, workouts, sleep patterns, or stress affect your glucose in real time, a CGM delivers the granular, continuous feedback that makes behavior change tangible. Athletes optimizing fueling strategies, individuals experimenting with dietary tweaks, or anyone curious about their metabolic patterns will find the density of data useful for spotting trends that single-point checks would miss.
On the other hand, if you want occasional validation - checking fasting glucose weekly, confirming stable readings after diet changes, or simply keeping tabs without the complexity of sensor application and smartphone syncing - a traditional meter offers simplicity, lower cost, and no learning curve. Budget is a real consideration: CGMs require ongoing sensor purchases and often subscription fees, while fingerstick meters involve only test strip costs and infrequent replacements.
Both approaches are tools for gathering insight, not diagnostic devices or substitutes for professional medical advice. Success with either method depends on setting clear, actionable goals before you start monitoring. Ask yourself what specific question you want the data to answer, how you'll use the information to adjust behavior, and whether the cost and effort align with the value you expect to gain. Glucose data becomes useful when it drives informed decisions about nutrition, activity, and recovery - not when it sits unreviewed in an app or creates unnecessary anxiety over normal fluctuations.
If you're unsure which path fits your situation, start with the simpler option and scale up only if your goals demand more detail. Monitoring is a means to an end, and the right choice is the one that keeps you engaged, informed, and moving toward the health outcomes you've defined for yourself.
Atrafen GLP Ultra GLP-1 Activator Diet & Weight Loss Supplement 60 Capsules
The Atrafen GLP Ultra GLP-1 Activator is a dietary supplement marketed to support GLP-1 pathways involved in glucose metabolism and appetite regulation. Unlike the continuous glucose monitors discussed earlier in this guide, this is not a monitoring device - it does not measure or track your glucose levels in real time.
This product comes in a 60-capsule bottle and is priced at $49.99. It holds a customer rating of 4.2 out of 5, suggesting generally positive user feedback, though individual results will vary. Because this is a supplement, its effects on glucose response and appetite depend on your unique metabolism, baseline diet, and activity patterns.
If you're exploring non-diabetic CGM use to understand how food and lifestyle influence your glucose, a supplement like this operates on a different level: it aims to influence metabolic pathways rather than provide direct data. Some people combine supplements with CGM tracking to see if they observe changes in glucose patterns, but supplements are not a substitute for the objective, time-stamped feedback a CGM provides.
Keep in mind that dietary supplements are not evaluated by the FDA for diagnosing, treating, or preventing disease. They may support wellness goals when paired with balanced nutrition and exercise, but they should not replace professional medical advice or glucose monitoring technology if you're using data to guide meaningful behavior change.
This supplement may appeal to those interested in metabolic health from multiple angles, but it is most useful when expectations are realistic: it complements, rather than replaces, tools like CGMs or guidance from a healthcare provider.
- ✅ Marketed to support GLP-1 pathways related to glucose and appetite
- ✅ 60-capsule supply at a mid-range price point
- ✅ Customer rating of 4.2 out of 5 suggests general satisfaction
- ⚠️ Does not measure or track glucose levels
- ⚠️ Individual results vary and are not guaranteed
- ⚠️ Not a substitute for direct glucose monitoring or medical guidance
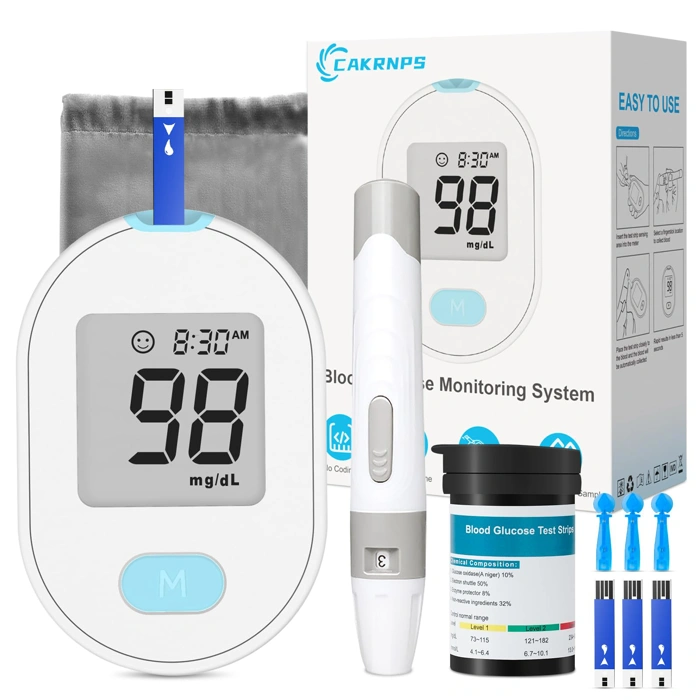
Blood Glucose Monitor Kit with 50 Strips & Lancets, No Coding, Auto Eject, 5-Second Results
For non-diabetics who want to check glucose levels occasionally - or validate trends seen in a CGM - this blood glucose monitor kit offers a low-cost, no-commitment alternative. Priced at $19.99, the kit includes 50 test strips, multipleancets, and a meter with no-coding setup, meaning you can start testing without programming the device for each new batch of strips.
The monitor delivers results in five seconds and features an auto-eject mechanism that removes used strips with the push of a button, reducing direct contact with blood samples. The kit provides everything needed to begin fingerstick testing immediately, making it suitable for spot-checking fasting glucose, post-meal levels, or comparing readings against a continuous monitor.
Because this is a traditional fingerstick system, each test requires a new strip and lancet. The included 50 strips support roughly seven weeks of daily testing or several months of occasional checks. There are no subscription fees, sensor-wear periods, or calibration windows - you test when you choose and pay only for additional strips as needed.
The no-coding feature simplifies use: insert a strip, apply a blood sample from a lanced fingertip, and read the result. The display is straightforward, with no app sync or trend graphs. For users exploring glucose variability without the cost or commitment of a CGM, or those who want a reference point to confirm sensor accuracy, this kit offers a practical entry point.
Keep in mind that fingerstick monitors capture single moments rather than continuous trends, and each test involves a finger prick. They're best suited for periodic checks rather than tracking real-time fluctuations throughout the day.
- ✅ No-coding setup - start testing immediately without device programming
- ✅ 5-second results with auto-eject feature for used strips
- ✅ Includes 50 strips and 50 lancets for $19.99
- ✅ No subscription fees or ongoing sensor costs
- ⚠️ Requires a finger prick for each test
- ⚠️ Provides single readings, not continuous trends
- ⚠️ 50-strip supply limited to occasional or short-term use
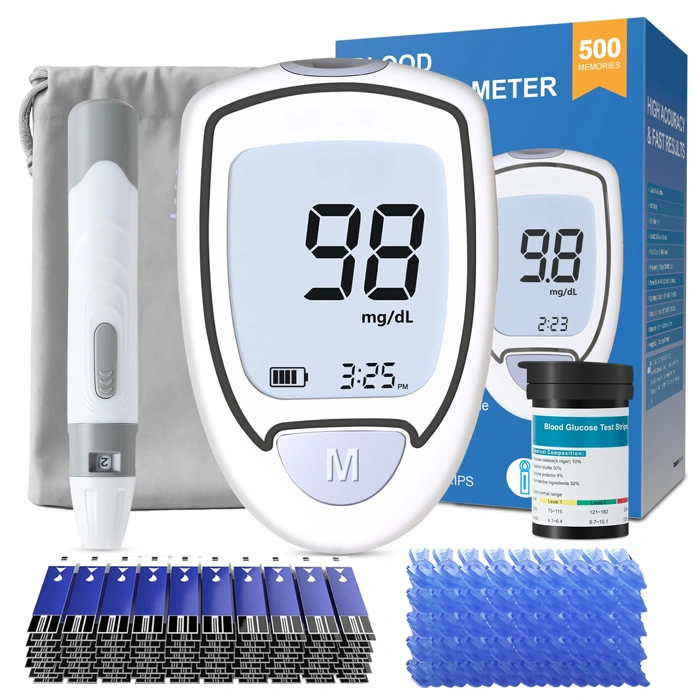
Glucose Monitor Kit with 50 Strips & Lancets, Auto Eject, No Coding, Large Display
This glucose monitor kit includes a meter with a large LCD display, 50 test strips, multipleancets, and an auto-eject lancing device. The no-coding feature means the meter is ready to use without manual calibration, and the larger screen makes it easier to read results at a glance.
The core fingerstick testing process works the same as other budget kits: you insert a strip, prick your finger, apply a blood sample, and get a reading in seconds. Where this kit may stand out is the display size - if you prefer larger numerals for quick checks in dim light or from different angles, the bigger screen can reduce squinting and make daily tracking feel less effortful.
The auto-eject lancing device is a convenience feature that releases the used lancet with a button press, cutting down on direct handling. For non-diabetic users testing once or twice a day to spot trends, this kit offers straightforward spot-checking without the upfront complexity of a continuous monitor.
Keep in mind that fingerstick monitors capture single moments rather than continuous curves. If you want to see how your glucose responds throughout a meal or overnight, a CGM will offer more granular insight. But if your goal is occasional verification - confirming fasting levels or checking post-meal peaks at predictable times - a fingerstick meter with a clear, easy-to-read display can be a practical and budget-friendly tool.
- ✅ Large LCD display for easier reading
- ✅ No-coding setup simplifies first use
- ✅ Auto-eject lancing device reduces direct lancet handling
- ✅ Includes 50 strips and 50 lancets in the kit
- ⚠️ Captures single snapshots rather than continuous trends
- ⚠️ Requires fingerstick for each reading
- ⚠️ Does not track glucose patterns between tests
Blood Sugar Glucose Monitor Kit with 50 Test Strips & Lancets, Auto Eject, Large LCD
The Blood Sugar Glucose Monitor Kit is the lowest-cost traditional glucose monitor in this guide at $14.56, and it includes everything needed to begin fingerstick testing: 50 test strips, multipleancets, a lancing device, and a carrying case. The large LCD display and auto-eject feature make it straightforward to use for users who prefer simplicity over connectivity or advanced logging.
This kit is designed for people who want to check glucose occasionally - perhaps after different meals or before and after exercise - without committing to a subscription or a continuous monitoring system. Because it includes 50 strips in the box, it provides enough tests to explore patterns over several weeks without an immediate need to purchase consumables separately.
The meter does not offer Bluetooth, app integration, or automatic data syncing. Results appear on the screen and must be logged manually if you want to track trends over time. That means more effort to spot patterns, but it also keeps the price low and the workflow uncomplicated for users who prefer a no-frills approach.
The auto-eject feature helps with hygienic strip disposal, and the large LCD is easier to read in varied lighting than smaller screens on some budget meters. The kit arrives ready to use, with the lancing device adjustable for comfort, though some users may still find fingerstick testing uncomfortable compared to sensor-based systems.
This monitor is best suited for users who are unsure whether regular glucose tracking will become part of their routine, or who want to validate initial patterns before investing in a continuous glucose monitor. It offers an accessible entry point for trial-and-error exploration of how specific foods, meal timing, or activity levels affect glucose, without the recurring sensor costs of CGM systems.
The tradeoff is clear: this kit exchanges convenience and real-time data for affordability and simplicity. It won't capture overnight trends or alert you to rapid changes, but it provides reliable spot checks at a price that makes testing less of a financial commitment.
- ✅ Lowest-cost option at $14.56 with 50 strips included
- ✅ Large LCD display and auto-eject feature
- ✅ No subscription or recurring sensor costs
- ✅ Complete kit with lancing device and carrying case
- ⚠️ No Bluetooth, app integration, or automatic data syncing
- ⚠️ Requires manual logging to track trends
- ⚠️ Fingerstick testing required for each reading
- ⚠️ Does not capture continuous or overnight glucose patterns
Key Questions to Ask Before Buying a CGM
- Do I have a specific behavioral or performance goal that benefits from continuous data?
- Am I prepared to interpret trends and adjust diet, exercise, or sleep accordingly?
- Does my budget accommodate sensor costs (typically $50 - $100+ per month)?
- Would occasional fingerstick testing provide enough insight at lower cost?
- Have I consulted a healthcare provider if I have prediabetic markers or metabolic concerns?
- Am I comfortable wearing a sensor continuously and managing device setup?